
Can Diabetes Cause Headaches? The Connection You Need to Know
Living with diabetes can bring a range of symptoms that affect daily life, and headaches are one of the more commonly reported concerns. Can diabetes cause headaches? In many cases, yes, blood sugar imbalances play a key role. Both low blood sugar (hypoglycemia) and high blood sugar (hyperglycemia) can interfere with normal brain function, which may lead to headaches.
Recognizing this connection is important for effective symptom management. Headaches related to diabetes are often associated with glucose fluctuations, dehydration, or changes in circulation. Noticing when headaches occur, and the symptoms that accompany them, can help determine whether blood sugar levels are the underlying cause.
“A diabetes-related headache is often the body’s silent alarm, signaling that your blood sugar balance needs immediate attention”
Understanding the Link Between Diabetes and Headaches
Diabetes does not directly cause headaches, but the changes it creates in the body may trigger them. The most common factor is unstable blood sugar:
- Low blood sugar (Hypoglycemia): The brain lacks sufficient energy, leading to sudden headaches.
- High blood sugar (Hyperglycemia): Dehydration and changes in circulation can cause dull, pressure-like headaches.
People with frequent blood sugar fluctuations may experience recurring symptoms, making consistent glucose control and timely management essential.
Not all headaches in people with diabetes are caused by blood sugar changes. Common causes such as tension headaches, migraines, dehydration, poor sleep, or stress should also be considered.

What Does a Diabetic Headache Feel Like?
Headaches from Low Blood Sugar (Hypoglycemia)
- Sudden, sharp, or throbbing pain
- Often accompanied by dizziness, sweating, shakiness, or confusion
Headaches from High Blood Sugar (Hyperglycemia)
- Dull, steady, pressure-like pain
- Linked with fatigue, thirst, or blurred vision
Tension-Like Headaches in Diabetes
- Tight, band-like pain around the forehead or temples
- Often triggered by stress, dehydration, or fluctuating blood sugar
High vs. Low Blood Sugar Headaches: Spotting the Key Differences
| Feature | Low Blood Sugar (Hypoglycemia) | High Blood Sugar (Hyperglycemia) |
|---|---|---|
| Onset | Sudden | Gradual |
| Headache Type | Sharp, throbbing | Dull, pressure‑like |
| Intensity | It can become severe quickly | Usually mild to moderate, persistent |
| Common Triggers | Skipping meals, excess insulin | Overeating, missed medication |
| Associated Symptoms | Sweating, shakiness, dizziness, confusion | Thirst, fatigue, blurred vision |
| Duration | Improves quickly after sugar intake | Lasts longer until glucose is controlled |
| Immediate Action | Consume fast‑acting carbohydrates | Hydrate and follow the prescribed treatment |
| Urgency Level | High. Needs quick correction | Moderate. Needs timely management |
← Swipe to see more →
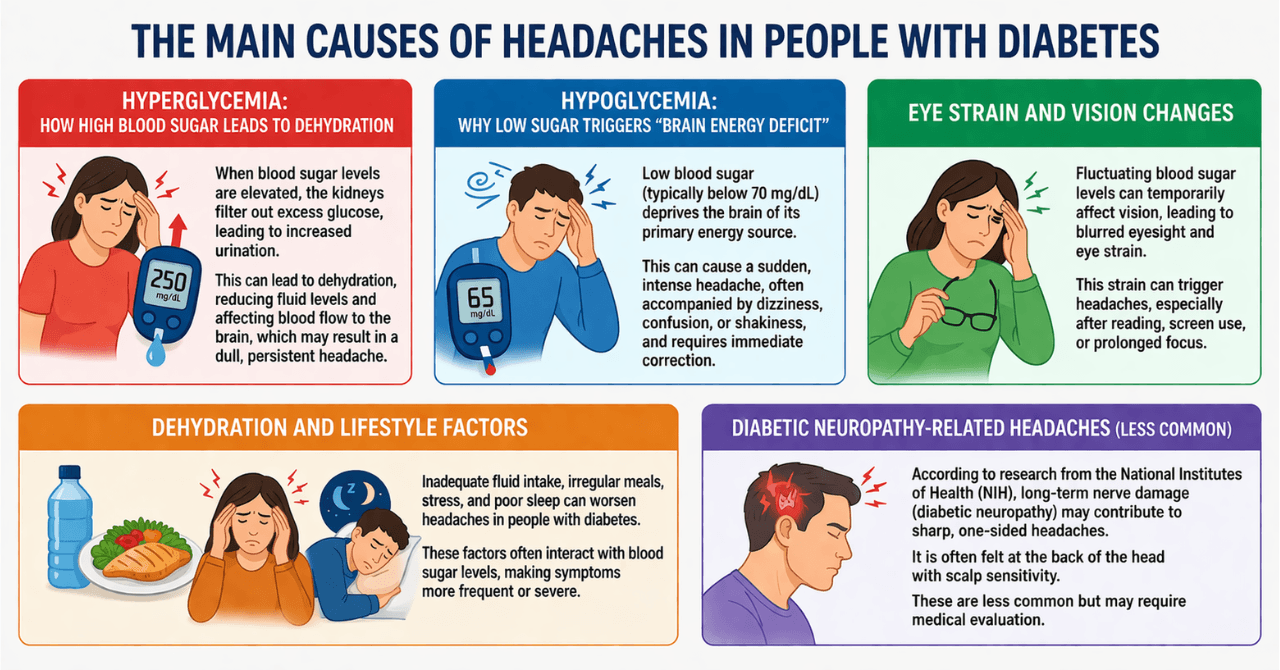
The Main Causes of Headaches in People with Diabetes
Below are the main causes of headaches in diabetes, most often linked to blood sugar imbalance and related physiological changes.
Hyperglycemia: How High Blood Sugar Leads to Dehydration
When blood sugar levels are elevated, the kidneys filter out excess glucose, leading to increased urination. This can lead to dehydration, reducing fluid levels and affecting blood flow to the brain, which may result in a dull, persistent headache.
Hypoglycemia: Why Low Sugar Triggers “Brain Energy Deficit”
Low blood sugar (typically below 70 mg/dL) deprives the brain of its primary energy source. This can cause a sudden, intense headache, often accompanied by dizziness, confusion, or shakiness, and requires immediate correction.
Eye Strain and Vision Changes
Fluctuating blood sugar levels can temporarily affect vision, leading to blurred eyesight and eye strain. This strain can trigger headaches, especially after reading, screen use, or prolonged focus.
Dehydration and Lifestyle Factors
Inadequate fluid intake, irregular meals, stress, and poor sleep can worsen headaches in people with diabetes. These factors often interact with blood sugar levels, making symptoms more frequent or severe.
Diabetic Neuropathy-Related Headaches (Less Common)
According to research from the National Institutes of Health (NIH), long-term nerve damage (diabetic neuropathy) may contribute to sharp, one-sided headaches. It is often felt at the back of the head with scalp sensitivity. These are less common but may require medical evaluation.
10 Warning Signs of Diabetes You Should Not Ignore
| Warning Sign | What It May Indicate |
|---|---|
| Frequent urination | Excess sugar in the blood increases urine output |
| Excessive thirst | Fluid loss due to frequent urination |
| Increased hunger | The body is unable to use glucose properly |
| Fatigue | Low energy due to poor glucose utilization |
| Blurred vision | Blood sugar affects eye fluid balance |
| Slow‑healing wounds | Poor circulation and reduced immune response |
| Unexplained weight loss | The body breaks down fat for energy |
| Frequent infections | High sugar weakens immunity |
| Tingling or numbness | Early nerve damage (neuropathy) |
| Recurring headaches | Blood sugar fluctuations |
← Swipe to see more →
Practical Steps: How to Treat and Prevent Diabetic Headaches
Managing diabetic headaches starts with correcting blood sugar levels quickly and maintaining long-term stability.
How to Treat Diabetic Headaches
1. Identify the Cause (Check Blood Sugar First)
- Low Blood Sugar: Follow the 15-15 rule: consume 15 g of fast-acting carbs, recheck after 15 minutes, repeat if needed.
- High Blood Sugar: Follow your healthcare provider’s instructions for all prescribed medications. Hydration supports overall health but does not replace medication adjustments.
2. Get Quick Symptom Relief
- Rest in a cool, dark, quiet room
- Use a cold compress (forehead) or a warm compress (neck)
- Only use OTC pain relievers under the guidance of a healthcare provider.
- Avoid NSAIDs if you have kidney problems or other complications.
- Never adjust prescribed medication on your own.
- Gentle massage of temples or neck
How to Prevent Diabetic Headaches
1. Keep Blood Sugar Stable
- Follow a consistent meal schedule
- Monitor glucose regularly (CGM or glucometer)
- Limit refined sugars and processed carbs
2. Improve Lifestyle Habits
- Stay hydrated
- Light, regular exercise (e.g., walking)
- 7–9 hours of sleep
- Manage stress with yoga, meditation, or deep breathing
- Track triggers in a headache diary
When to See a Doctor
Seek medical attention if headaches are:
- Frequent, severe, or persistent
- Accompanied by confusion, fever, or vision changes
- Associated with high ketone levels (>1.5 mmol/L) or blood sugar >300 mg/dL
Clinical Evidence: Diabetes and Headaches
| Study / Source | Key Findings |
|---|---|
| PubMed: Migraine and Type 2 Diabetes (2016) | Metabolic instability and frequent glucose fluctuations were associated with higher headache prevalence in diabetes patients. |
| Systematic Review: Diabetes & Headache Meta‑Analysis (2024) | Glucose swings contribute to headache onset; both hypoglycemia and hyperglycemia were linked to increased headache risk. |
| ADA Clinical Guidelines / Case Observations (2023) | Severe hyperglycemia can trigger headaches in some patients; maintaining glucose stability is key for prevention. |
← Swipe to see more →
These findings are based on peer‑reviewed studies and clinical guidelines.
Final Thoughts on the Link Between Diabetes and Headaches
Diabetic headaches are usually caused by blood sugar fluctuations, whether too low or too high. Monitoring glucose levels, staying hydrated, eating balanced meals, exercising, and managing stress can prevent or reduce headaches. Identifying personal triggers and consulting healthcare professionals ensures safer, more effective management for long-term well-being.
At Polar Bear Meds, we understand that managing your health and medications can sometimes be challenging. As a licensed Canadian pharmacy, we provide high-quality medications and reliable support to help you stay on track. You can conveniently order online from Canada with secure delivery to the U.S., making your treatment easier and more consistent.
Important Disclaimer: Polar Bear Meds is a licensed Canadian pharmacy providing secure online medication delivery to the U.S. This article is for informational purposes only & does not replace professional advice. Always consult a licensed healthcare professional/doctor before making changes to your diabetes treatment, medication, or lifestyle.
Frequently Asked Questions
Yes. Both high & low blood sugar can trigger headaches and dizziness. Low sugar deprives the brain of energy, causing sudden headaches and lightheadedness. High sugar can lead to dehydration and sluggish circulation, resulting in dull, persistent headaches and imbalance.
Yes. Hyperglycemia often causes dull, pressure-like headaches. High glucose levels may lead to dehydration and affect blood flow, making headaches more likely until blood sugar is controlled.
Seek medical attention if headaches are frequent, severe, or persistent, or if they occur alongside confusion, vision changes, fever, or high ketone levels. Immediate evaluation is important to prevent complications.
It’s possible if blood sugar is frequently unstable. Recurring headaches often signal glucose fluctuations, dehydration, stress, or other diabetes-related factors. Consistent monitoring and lifestyle management can help reduce daily headaches.




