
Long-Term Side Effects of Insulin Overdose in the Body: What You Need to Know
Insulin overdose is a serious medical emergency that can cause dangerously low blood sugar and immediate life-threatening complications. But many patients and caregivers ask: Can a single overdose or repeated smaller episodes leave permanent damage in the body? While immediate treatment can restore normal blood sugar levels, it may not fully prevent long-term effects, particularly after severe or repeated episodes.
Severe or repeated overdoses may lead to cognitive impairment, hypoglycemic encephalopathy, heart rhythm disturbances, and other long-term metabolic changes. Understanding the potential long-term effects of an overdose of insulin is critical for patients and caregivers to manage risks and support recovery effectively.
Immediate Consequences vs. Long-Term Complications of Insulin Overdose
When an insulin overdose occurs, the body enters a state of acute stress. Knowing what happens immediately versus what may occur later is essential for effective treatment and recovery.
Immediate Consequences (Acute Phase) of Insulin Overdose
The most urgent effect is a rapid drop in blood glucose, causing severe hypoglycemia. Organs, especially the brain, are deprived of energy almost instantly.
- Common Symptoms: Shakiness, sweating, intense hunger, confusion, blurred vision.
- Critical Risks: If untreated within minutes, hypoglycemia can escalate to seizures, loss of consciousness (insulin coma), or death.
According to PubMed Central (PMC8955302), rapid intervention with glucose or Glucagon is vital to prevent permanent damage.
Long-Term Complications (Aftermath) of Insulin Overdose
Even after glucose levels normalize, lingering effects may persist, affecting cognitive, cardiovascular, and neurological health.
- Cognitive Impact: Memory gaps, brain fog, or lasting cognitive impairment (hypoglycemic encephalopathy).
- Systemic Stress: The adrenaline surge during overdose can strain the heart and nervous system, potentially causing arrhythmias or hypoglycemia unawareness in future episodes.
- Other Risks: Repeated severe lows may lead to chronic neurological or metabolic complications.
As reported in PubMed Central (PMC3424500), severe or repeated insulin overdoses can cause lasting deficits despite initial recovery.
Quick Comparison: Immediate vs. Long-Term Effects of Insulin Overdose
| Feature | Immediate Consequence | Long-Term Side Effect |
|---|---|---|
| Primary Cause | Sudden blood glucose drop | Prolonged metabolic stress |
| Main Symptom | Seizures, fainting, sweating | Memory loss, arrhythmias, nerve damage |
| Treatment | Emergency glucose/Glucagon | Specialist care, monitoring, lifestyle adjustments |
← Swipe to see more →
Long-Term and Lasting Effects of Insulin Overdose
Severe insulin overdoses can leave lasting effects that extend beyond the acute hypoglycemic episode. These complications are primarily categorized into neurological, cardiovascular, and sensory consequences. They may persist for months or even become permanent, depending on the severity of the overdose and the timeliness of treatment.
Neurological Damage (Hypoglycemic Encephalopathy)
Prolonged low blood sugar starves the brain of glucose, potentially causing hypoglycemic encephalopathy. This can result in:
- Permanent cognitive impairment, including memory loss and difficulty concentrating
- Motor skill deficits and impaired coordination
- Chronic “brain fog” that persists despite normal blood glucose levels
- Increased risk of long-term seizures in cases of repeated or severe hypoglycemia
According to a study published in PubMed Central, severe insulin overdose can lead to permanent neurological damage.
Cardiovascular Complications
A massive insulin overdose triggers a surge of counter-regulatory hormones like adrenaline, placing extreme stress on the heart. Long-term effects may include:
- Arrhythmias or irregular heartbeats
- Stress-related cardiomyopathy and weakened cardiac muscle
- Higher risk of cardiac events in patients with pre-existing heart conditions
Research from NIH sources shows that some individuals may develop long-term arrhythmias or weakened cardiac function, especially those with pre-existing heart conditions.
Sensory Effects and Hypoglycemia Unawareness
The nervous system may recalibrate after a severe overdose, impairing the body’s ability to sense low blood sugar:
- Reduced early warning signals such as shaking, sweating, or palpitations
- Increased danger in future hypoglycemia events due to delayed recognition
- This nerve desensitization creates a dangerous cycle, making future insulin management significantly more challenging and unpredictable
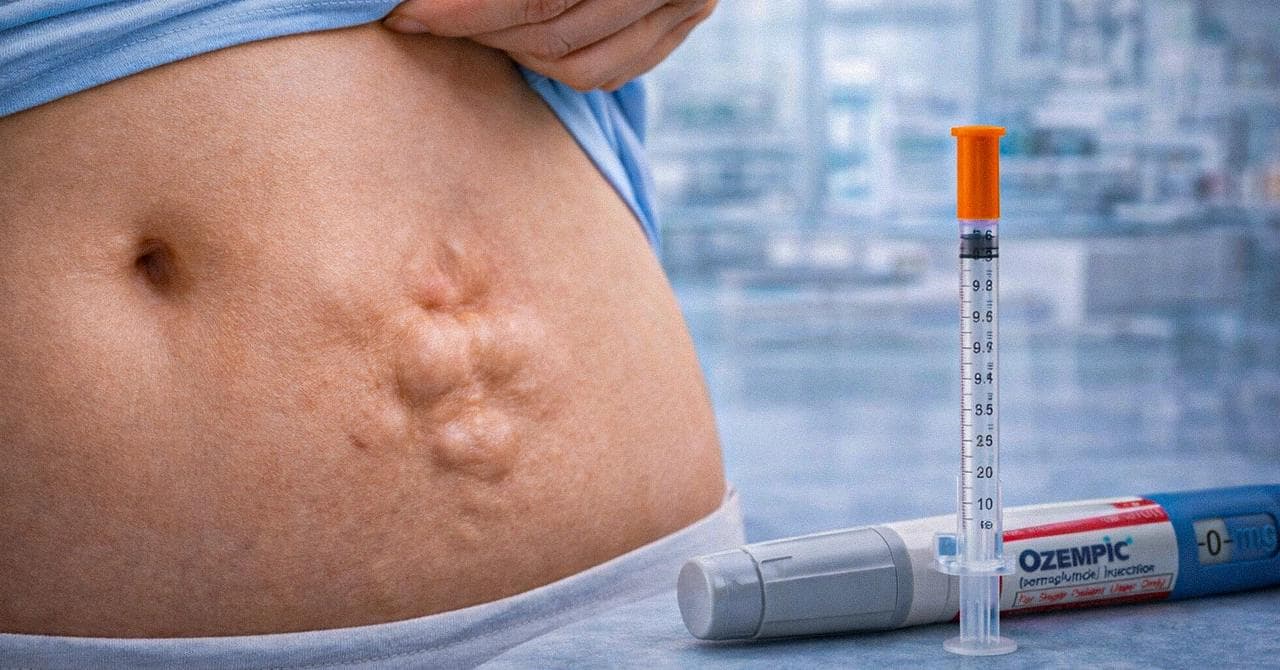
Physical Tissue Changes (Lipodystrophy)
High-volume insulin injections in a single site can cause localized tissue changes:
- Permanent dents, lumps, or abnormal fat growth at injection sites
- Potentially unpredictable insulin absorption in the future, complicating glucose control
Recovery vs. Permanent Damage: When is an Insulin Overdose Serious?
| Factor | Full Recovery Potential | Permanent Damage / Serious Outcome |
|---|---|---|
| Duration of Hypoglycemia | Glucose restored within minutes; unconsciousness typically lasts <30 mins. | Prolonged hypoglycemia (>60-90 mins) can lead to irreversible neuronal death (hypoglycemic encephalopathy). |
| Cognitive Symptoms | Short-term brain fog, shakiness, or confusion that resolves within 24-48 hours. | Persistent memory loss, cognitive impairment, motor skill deficits, or personality changes. |
| High-Risk Variables | Prompt treatment, short-acting insulin, and younger or otherwise healthy patients. | Delayed treatment, long-acting insulin, elderly/frail patients, alcohol or drug use. |
| Medical Treatment | Oral fast-acting carbohydrates or a single dose of Glucagon; close monitoring. | Extended IV Dextrose therapy, ICU monitoring, and long-term neurological care. |
| Recovery Probability | >95% in cases with timely intervention and mild-to-moderate hypoglycemia. | 1-3% in hospital-admitted severe cases; risk increases if intervention is delayed >2 hours. |
| Immediate Action | Consume 15-20g fast-acting carbs; monitor blood sugar for 24 hours. | Call 911 immediately, administer Glucagon if available; hospital monitoring mandatory. |
← Swipe to see more →
Risk Factors for a Severe or Fatal Insulin Overdose
The risk of severe consequences depends on several key factors, including the type of insulin, health status, timing, and other contributing conditions.
Factors That Increase the Risk of Severe or Lasting Effects from an Insulin Overdose
Type of Insulin
- Rapid-acting: Fast drop but shorter duration; easier recovery with prompt treatment.
- Long-acting/basal: Can stay active 24-42 hours, causing repeated lows and a higher risk of long-term effects.
Concurrent Substance Use
- Alcohol: Blocks liver glucose release, worsening hypoglycemia.
- Beta-blockers: Mask warning signs like shakiness or palpitations.
Health Status
- Kidney or liver impairment: Slows insulin clearance, prolonging low blood sugar.
- Age and frailty: Older adults respond more slowly to hypoglycemia; they are at a higher risk of heart complications.
Timing of Overdose
- During sleep, hypoglycemia can go unnoticed for hours, increasing the risk of brain damage.
Accidental or Preventable Causes
- Double-dosing or wrong insulin type/dose.
- Skipping meals or intense exercise without adjusting insulin.
- Misreading pen/syringe markings (common in the elderly or the visually impaired).
Intentional or High-Risk Situations
- Suicide attempts or self-harm.
- Cognitive impairment, dementia, or severe psychiatric conditions.
- High-risk populations: children with Type 1 diabetes, elderly patients.
Indicators of Serious Outcomes
- Large total insulin dose.
- Delayed treatment (>60-90 minutes for severe lows).
- Development of complications such as hypoglycemic encephalopathy or cardiac issues.

Conclusion: Managing Long-Term Side Effects of Insulin Overdose
Insulin overdose can lead to lasting effects if not treated promptly, impacting brain and heart health. While most people recover fully, early intervention and proper follow-up care are key to preventing long-term complications. Staying aware of symptoms, managing insulin carefully, and consulting healthcare providers may help ensure a safe and stable recovery.
Frequently Asked Questions
Severe or repeated insulin overdose can lead to long-term effects such as memory loss, cognitive impairment, and hypoglycemic encephalopathy (brain injury). It may also cause heart rhythm disturbances and hypoglycemia unawareness, increasing the risk of future complications. Most effects occur due to prolonged low blood sugar, depriving the brain of glucose.
Yes. Most people (over 90%) recover fully if treated quickly with glucose or glucagon. However, delayed treatment or severe, prolonged hypoglycemia can lead to permanent neurological damage or, rarely, death.
It depends on the type:
- Rapid-acting insulin: approximately 3-5 hours
- Short-acting: approximately 6-8 hours
- Long-acting (e.g., glargine, degludec): up to 24-42 hours or longer, which can cause prolonged or repeated hypoglycemia after overdose.
Yes, but it is rare. Permanent brain damage can occur if blood sugar remains critically low for an extended period (typically >60-90 minutes in severe cases), leading to hypoglycemic encephalopathy.
- Immediately check your blood sugar
- Consume 15-20 g of fast-acting carbohydrates (juice, glucose tablets)
- Monitor levels frequently for several hours
- Seek medical help or call 911 if symptoms worsen (confusion, seizures, unconsciousness)
Medical Disclaimer
This blog is for informational purposes only and does not replace professional medical advice. Information about insulin overdose and its long-term effects may not apply to every individual, as outcomes can vary based on health status and circumstances. Always seek guidance from a licensed healthcare provider or endocrinologist for any concerns, symptoms, or treatment decisions. In case of a medical emergency, call 911 immediately.




