
What Is the Difference Between Regular and NPH Insulin?
NPH (Neutral Protamine Hagedorn) insulin is an intermediate-acting insulin designed to provide background blood sugar control throughout the day and night. It typically begins working within 1-2 hours and peaks between 4-12 hours, making it commonly used for managing fasting glucose levels, especially overnight. Due to its pronounced peak effect, NPH can be less predictable compared to newer long-acting insulin analogs.
In contrast, Regular insulin is a short-acting insulin used primarily for mealtime blood sugar control. It starts working within 30-60 minutes and peaks in 2-4 hours, helping manage post-meal glucose spikes. Understanding these distinct timing patterns is the key to selecting an insulin strategy that fits your unique daily lifestyle and glucose patterns.
Major Differences Between Regular and NPH Insulin
The primary distinction between these two insulins lies in their biological roles and formulation. Regular insulin functions as a “bolus” insulin, designed to manage immediate glucose needs around meals. NPH insulin acts as a “basal” insulin, helping maintain steady blood sugar levels between meals & overnight.
Visually, they are also easy to differentiate. Regular insulin is a clear, uniform solution that does not require mixing. NPH insulin appears cloudy due to the addition of protamine, a protein that slows its absorption and extends its action. Because of this suspension, NPH must be gently rolled before use to ensure even distribution, unlike Regular insulin, which is ready to use. These differences in structure and function are why both are often used together in a basal-bolus regimen for more balanced glucose control.
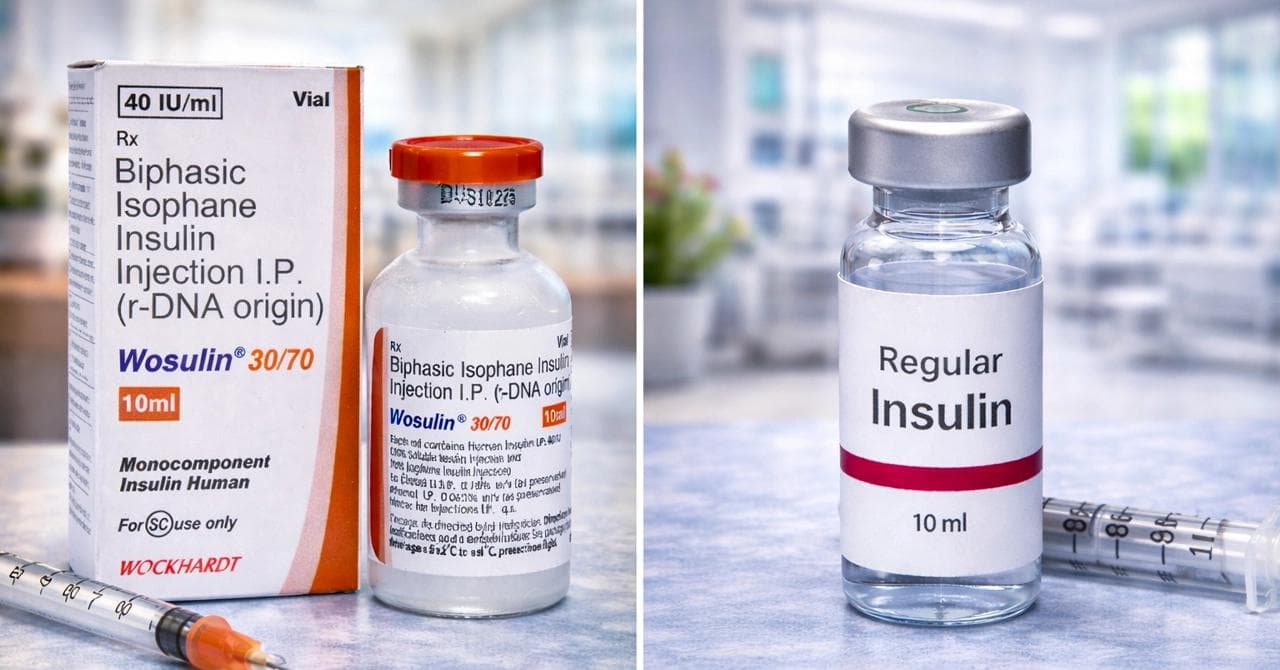
Why Regular Insulin Is Clear, and NPH Insulin Is Cloudy
The difference in appearance reflects how each insulin is formulated and how it is designed to act in the body. Regular insulin is a fully dissolved, uniform solution. It contains no added substances to slow its absorption, allowing the insulin molecules to remain freely mixed in the liquid. This is why it appears clear and transparent.
NPH insulin, in contrast, is a suspension rather than a true solution. It contains added protamine and zinc, which bind with insulin molecules to form small particles within the liquid. These particles do not fully dissolve, giving NPH its characteristic cloudy or milky appearance.
These particles are part of the formulation that allows NPH to release insulin more gradually after injection. Because they naturally settle at the bottom of the vial over time, NPH insulin must be gently rolled before use to evenly redistribute the suspension and ensure consistent dosing.
Onset, Peak Times & When to Inject Regular vs. NPH Insulin
Based on clinically accepted ranges from organizations like the American Diabetes Association (ADA).
| Feature | Regular Insulin (Short-Acting) | NPH Insulin (Intermediate-Acting) |
|---|---|---|
| When to Inject | ~30 minutes before meals | Morning and/or bedtime |
| Onset | 30-60 minutes | 2-4 hours |
| Peak | 2-4 hours | 4-12 hours |
| Duration | 5-8 hours (up to ~10) | 12-18 hours (sometimes longer) |
| Role | Mealtime (bolus) control | Background (basal) control |
| Hypoglycemia Risk | 2-4 hours after dose | 4-12 hours after dose |
← Swipe to see more →
How to Time Regular and NPH Insulin
Regular insulin (mealtime use)
- Inject about 30 minutes before eating
- Matches the post-meal rise in blood sugar
- Taking it too close to or after a meal can lead to early spikes
NPH insulin (basal use)
- Taken on a fixed schedule (once or twice daily)
- Common timings:
- Morning dose: daytime coverage
- Bedtime dose: overnight and fasting control
- Not meal-based, but it can lower blood sugar several hours later, especially if meals are delayed or skipped
Always follow your healthcare provider’s instructions, as timing and dosing may vary.
How to Mix Regular and NPH Insulin in One Syringe
Step 1: Prepare both vials
Wash your hands thoroughly, then wipe the tops of both vials with an alcohol swab. Gently roll the NPH (cloudy) vial between your palms to mix it evenly. Do not shake, as this may create bubbles & affect dosing accuracy.
Step 2: Add air to the NPH (cloudy) vialDraw air into the syringe equal to the prescribed NPH dose. Inject this air into the NPH vial without withdrawing any insulin. Then remove the needle.
Step 3: Add air to the Regular (clear) vialDraw air into the syringe equal to the Regular dose, then inject it into the Regular vial.
Step 4: Draw Regular insulin firstInsert the needle into the Regular vial, turn it upside down, and withdraw the exact prescribed dose of clear insulin.
Step 5: Draw NPH insulin secondInsert the needle into the NPH vial, turn it upside down, and slowly withdraw the required NPH dose into the same syringe.
Important safety note (No push-back rule): Do not push insulin back into the NPH vial if you withdraw too much. Once Regular insulin is already in the syringe, pushing it back can contaminate the vial and affect future doses. If an error occurs, discard the syringe and start over.

Low Blood Sugar Risks with Regular vs. NPH Insulin
Evidence from clinical literature indexed in PubMed Central and PubMed indicates that hypoglycemia risk differs mainly in relation to peak action, duration, and timing.
NPH Insulin (Intermediate-Acting)
- Higher risk of nocturnal hypoglycemia, especially with evening or bedtime dosing.
- Strong peak effect (4-10 hours) can occur during sleep.
- More variable absorption, increasing unpredictability of lows.
- Studies in PubMed Central (PMC1994862, PMC12547051) report a higher overall hypoglycemia risk compared with modern basal analogs.
Regular Insulin (Short-Acting)
- Higher risk of post-meal hypoglycemia if food intake is delayed or reduced after injection.
- Peak action occurs in 2-4 hours, aligning with meal-related glucose changes.
- Requires consistent meal timing to avoid a mismatch between insulin action and glucose intake.
- Risk increases if doses are stacked too closely, leading to late-afternoon or evening hypoglycemia due to overlapping action.
Overall: NPH hypoglycemia is more nocturnal and unpredictable, while Regular insulin hypoglycemia is more timing-dependent and meal-related.
Can You Substitute Regular Insulin for NPH Insulin?
No, Regular insulin and NPH insulin cannot be directly substituted for each other because they have fundamentally different pharmacokinetic profiles and clinical roles. As noted in the PubMed Central (NCBI Bookshelf, NBK549860), NPH is an intermediate-acting basal insulin, while Regular insulin is short-acting and used for mealtime control. Because their onset, peak, and duration differ, switching between them without appropriate dose adjustment can lead to hypoglycemia or hyperglycemia and poor glucose control.
Comparison Table: Regular (R) vs. NPH (N) Insulin
| Feature | Regular Insulin (R) | NPH Insulin (N) |
|---|---|---|
| What is it | Short-acting, mealtime insulin | Intermediate-acting, basal insulin |
| Visual Appearance | Crystal clear solution | Cloudy/milky suspension |
| Primary Role | Controls post-meal glucose spikes | Maintains baseline (between meals & overnight) |
| Mixing Order | Draw first (clear before cloudy rule) | Draw second |
| Resuspension | Not required | Must be gently rolled before use |
| Storage (In Use) | Stable at room temperature (~28 days) | Stable at room temperature (~28 days) |
| Exercise Impact | Rapid glucose drop if active near peak | Prolonged glucose-lowering effect due to longer action |
| Key Consideration | Timing must match meals closely | Peak can affect fasting or overnight glucose levels |
← Swipe to see more →
Conclusion: Choosing the Right Balance Between Regular and NPH Insulin
Regular and NPH insulin work together to provide complete blood sugar control, but serve very different roles. Regular insulin manages rapid post-meal glucose spikes, while NPH insulin provides longer background coverage between meals and overnight. Understanding their differences in timing, peak action, and risk patterns helps ensure safer and more effective diabetes management. When used correctly under medical guidance, this combination supports better overall glucose stability throughout the day.
Frequently Asked Questions
Yes. Humulin R and Novolin R are brand names of Regular (short-acting) insulin. They contain the same type of active insulin and are used for mealtime blood sugar control.
Accidentally taking NPH instead of Regular insulin may cause delayed or mismatched glucose control, leading to hypoglycemia or hyperglycemia. Monitor blood sugar closely and contact a healthcare provider immediately.
In the U.S., some human insulins like Regular and NPH may be available without a prescription in certain states, but availability varies, and medical supervision is still strongly recommended.
To prevent contamination. If NPH (cloudy) is drawn first, it can contaminate the Regular vial and alter its action. “Clear before cloudy” ensures accuracy and safety.
Yes. Unopened insulin should be refrigerated. Once in use, it can usually be kept at room temperature for about 28 days, depending on product instructions.
Yes, Regular insulin and NPH insulin can be mixed in the same syringe, but only if prescribed by a healthcare provider and using the correct technique. Regular (clear) insulin is always drawn first, followed by NPH (cloudy) insulin to avoid contamination. Always follow proper injection instructions and never mix insulins unless you’ve been specifically trained to do so.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Information regarding Regular and NPH insulin may vary based on individual health conditions. Always consult a qualified healthcare provider or diabetes specialist before starting, stopping, or changing any insulin therapy.




